Contents
As in all other organisms reproduction is the formation of new individuals of the same species. Sexual reproduction is the only method of reproduction in our species. Sexual reproduction involves the fusion of specialised haploid sex cells. The fusion of sperm and egg cell is called fertilisation. Fertilisation results in the formation of a diploid zygote from which a new individual develops.
Reproductive Structures
Both the male and female reproductive structures have 3 levels of organisation:
1. Production of sex cells.
2. Transport tubes.
3. Glands to secrete hormones.
The Male Reproductive System
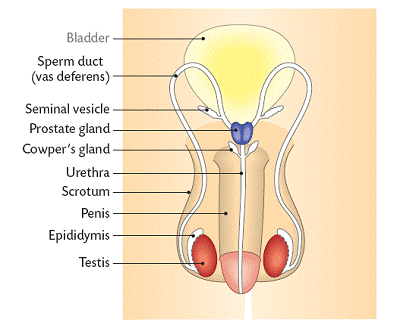
The gonad is the name for the organ that produces sex cells in organs. The male gonads are called the testes.
The testes are contained in the scrotum.
The testes produce the sperm cells by meiosis. The temperature must be lower than body temperature for this to occur. There are tubules that are lines with sperm producing cells. Testosterone, the male sex hormone, is also produced in the testes. Once the sperm are produced they mature in the epidymis. This structure is located outside of the testis. If they are not released within about 6 weeks they are broken down and released to the bloodstream by a process called resorption. The sperm are carried to the urethra by the sperm duct. The urethra carries both sperm and urine.
The sperm cells are carried within a liquid called semen. The semen is produced by the seminal vescicles, the
prostate gland, and Cowper’s glands. The semen also contains nourishment for the sperm cells.
Sperm cells are released by ejaculation. About 50-300 million sperm cells are released at one time.
Sperm cells, also called spermatozoa, are haploid containing 23 chromosomes. Their production begins at puberty.
The penis is adapted to place sperm cells into the female. The tip is called the glans. Erection occurs when blood rushes into the penis.
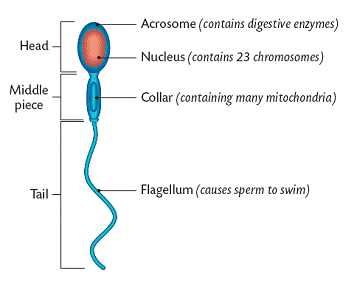
THE STRUCTURE OF THE SPERM CELL
MALE HORMONES
Male hormones are produced by the pituitary gland during puberty. They are:
FSH- Follicle Stimulating Hormone: This causes the production of sperm by meiosis.
LH- Leuteinising Hormone: Stimulates the testes to produce testosterone.
TESTOSTERONE
During the period of pregnancy testosterone causes the development of primary male sex characteristics. These include the development of the penis and the other male reproductive parts.
Later in life, at puberty, testosterone causes the enlargement of the reproductive parts as well as the development of secondary sexual characteristics. These are characteristics that distinguish males from females.
Male secondary sexual characteristics included:
1. hair growth on the face, underarm, chest and pubic region
2. enlarged larynx producing a deeper voice
3. wider shoulders
4. greater skeletal muscular development
5. growth in height and weight
MALE INFERTILITY
The most common cause of male infertility is the low production of sperm. There are many causes of low sperm production. Stress, alcohol and drug abuse, high temperature of the testes, and low testosterone production are all causes.
THE FEMALE REPRODUCTIVE SYSTEM
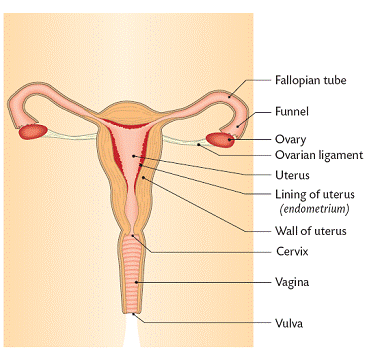
OVARIES
Ovaries produce eggs and female hormones. At puberty there are about 40,000 diploid eggs. Each egg is enclosed in a group of cells called a follicle. About 20 haploid eggs are produced each month. Usually all but one die. The haploid egg cell is called the ovum and is surrounded by the Graafian follicle which produces the female hormone called oestrogen. Ovulation is the release of the egg from the follicle. This occurs when the follicle bursts.
FALLOPIAN TUBES
The fallopian tubes are about 12 cm long and have ends that are funnel shaped. These ends collect the egg after ovulation. Cilia and peristalsis move the egg along the tube. The egg will die in the tube if it is not fertilised.
UTERUS
The uterus, also known as the womb, is made of involuntary muscle. It is lines with the endometrium. This lining thickens with cells and blood every month. This happens in order to nourish the embryo (if present). The opening of the uterus is called the cervix.
VAGINA
The vagina is a muscular tube which allows the sperm to enter the female as well as the baby to exit. It is lined with mucous secreting cells. The urethra opens near the vagina. The vagina is protected by folds of skin called the vulva. The hymen partially blocks the entrance of the vagina. It is broken by sexual intercourse or with the use of tampons.
THE MENSTRUAL CYCLE

The menstrual cycle occurs every 28 days from puberty to menopause (the end of the females reproductive life). It occurs only if fertilisation of the egg has not taken place.
The typical events of the menstrual cycle are:
Day 1 to day 5-
a. The endometrium breaks down and is shed from the body. This is called menstruation.
b. Meiosis occus in the ovary to produce a new egg surrounded by the Graafian follicle.
Day 6 to day 13-
a. Oestrogen is produced by the Graafian follicle. Oestrogen also stimulates the endometrium to thicken again. One Graafian follicle with one egg develops.
b. Oestrogen stimulates the production of LH (leuteinising hormone)
Day 14-
a. The surge of LH stimulates ovulation.
b. The egg enters the funnel of the Fallopian tube. It can be fertilised for the next 48 hours.
Day 15 to day 26-
a. The corpus luteum (yellow body) develops from the remains of the Graafian follicle. This produced progesterone and some oestrogen. The progesterone causes the endometrium to continue to thicken. It also prevents new eggs from forming.
b. The egg that was released at day 14 will die if it is not fertilised.
c. If fertilisation did not take place the corpus luteum begins to degenerate.
Day 26 to day 28-
a. Oestrogen and progesterone levels decline.
b. The endometrium begins to break down.
c. Day one of the cycle begins.
FEMALE HORMONES
In summary:
Endometrium thickened by oestrogen in days 1-14 and by progesterone in days 15-28.
Both prevent egg development.
At puberty, oestrogen causes the primary female sexual characteristics of the growth of the sex organs. At puberty both oestrogen and progesterone cause the secondary female characteristics.
They include:
a. The enlargement of the breasts
b. Widening of the hips
c. Increased body fat
d. Growth of public and underarm hair
e. General growth spurt in height
|
HORMONE |
SITE OF PRODUCTION |
TIME OF PRODUCTION |
FUNCTIONS
|
|
FSH-follicle stimulating hormone |
Pituitary Gland |
Days 1-5 of menstrual cycle |
Stimulates egg production within Sometimes used in fertility Graafian follicles secrete
|
|
Oestrogen |
Graafian follicle |
Days 5-14 of menstrual cycle |
Development of endometrium. Inhibits FSH so no new eggs Stimulates the release of LH |
|
LH- leuteinising hormone |
Pituitary Gland |
Day 14 of menstrual cycle |
Causes ovulation. Causes Graafian follicle to develop |
|
Progesterone |
Corpus luteum |
Days 14-28 of menstrual cycle
|
Maintains endometrium. Inhibits FSH so no new eggs Inhibits LH so no new ovulations Prevents contractions of the uterus. |
FEMALE INFERTILITY
Female infertility is the inability to conceive either by fertilisation failure or implantation failure. Egg cell formation or ovulation may not occur due to a hormone imbalance. The egg cell may not be able pass to the uterus due to blockage of the Fallopian tubes. Treatment with hormones may be successful. In-vitro fertilisation and implantation is often used to treat female infertility.
FIBROIDS
Fibroids are benign tumours of the uterus. They are slow growing and range in size. Small fibroids produce no symptoms while large ones can cause heavy and prolonged menstrual bleeding. They can also cause pain, miscarriage, or infertility. Some science shows that they may be caused as an abnormal response to oestrogen. Large fibroids are removed by surgery. In severe cases where there are many large fibroids the uterus may have to be removed. This is called a hysterectomy.
COPULATION
Copulation is also called coitus or sexual intercourse. During this process the penis moves into the vagina in order to deposit semen which contains sperm cells. The depositing of the semen is called insemination.
FERTILISATION
a. After insemination the sperm will move up the Fallopian tubes.
b. If ovulation has occurred and an egg is present the egg will release a chemical that attracts the sperm. This is called chemotaxix.
c. The sperm that reaches the egg will use an enzyme in its acrosomes to make an opening in the membrane of the egg.
d. Once one sperm enters the egg (only the head enters) the egg forms a membrane that prevents other sperm from entering.
e. The nucleus of the egg fuses with the nucleus of the egg. A diploid zygote forms.
f. Fertilisation may take place during days 11-16 of the menstrual cycle.
EVENTS OF FERTILISATION


IMPLANTATION
About 6-9 days after fertilisation the fertilised egg becomes embedded into the lining of the uterus. The zygote has now become an embryo. A membrane called the amnion develops around the ebbryo. This membrane will secrete amnion fluid which surrounds and protects the embryo.
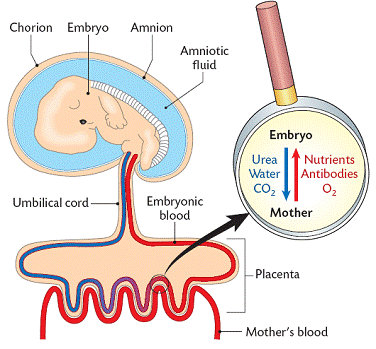
PLACENTA FORMATION
a. After implantation the embryo forms another membrane called the chorion. This surrounds the embryo.
b. Projections of the chorion called villi join with blood vessels in the endometrium to form the placenta.
c. The placenta become fully functional in about 3 months.
d. The umbilical cord connects the embryo (at the navel) with the placenta.
FUNCTIONS OF THE PLACENTA
1. Protection of the Embryo:
A. It hinders the entry of pathogens from the mother.
B. It allows the entry of antibodies from the mother (passive induced immunity).
C. It keeps the embryo separated from the mothers higher blood pressure.
D. It prevents exchange of red blood cells avoiding the deadly possibility of agglutination
2. Gas Exchange:
A. It supplies O2 from the mother.
B. It excretes CO2 from the embryo to the mothers blood.
3. Nutrient Supply:
Glucose, amino acids, lipids, vitamins and minerals pass to the embryo from the mothers blood.
4. Endocrine:
It secretes a variety of hormones including oestrogen and progesterone. The hormones maintain the pregnancy and prepare the mothers body for birth and lactation.
5. Excretion:
Metabolic wastes, CO2 and urea, pass from embryo into the mothers blood.
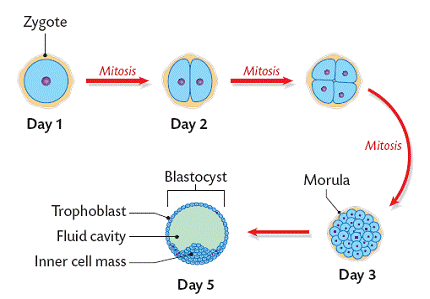
EARLY DEVELOPMET OF THE ZYGOTE (higher level)
1. The zygote divides many times by cleavage (increase in the number of cells by division but no overall increase in size) to double its cell number. A solid clump of about 100 cells called the morula is formed.
2. About 5 days after fertilisation the morula develops into a hollow ball called a blastocyst. The outer cells of the blastocyst form the trophoplast. This will become the membranes around the embryo. The inner cells, called the inner mass will become the embryo.
3. The blastocyst is pushed down the fallopian tube and into the uterus for implantation.
In normal development the sperm fertilizes the egg. The cortical reaction occurs raising the fertilization membrane and cell divisions occur until the blastula stage. When the embryo reaches the blastula stage the embryo releases an enzyme that dissolves the fertilization membrane and the young embryo swims free to continue development.

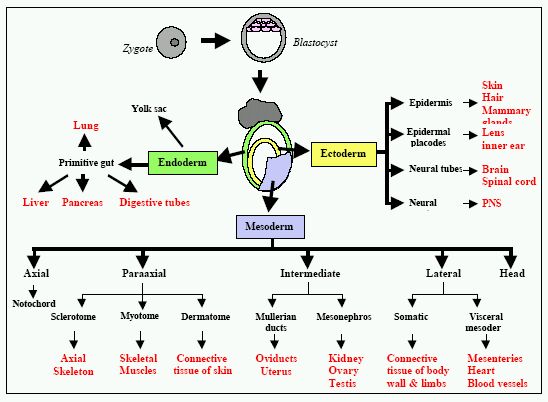
DEVELOPMET OF THE EMBRYO (higher level)
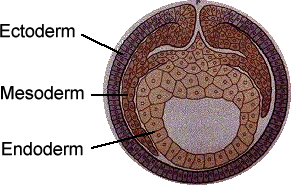
The mesoderm cells further develop into the muscles and blood, the endoderm develops into the digestive tract and lungs, and the ectoderm develops into the skin, nerves and brain.
WEEK TO WEEK DEVELOPMENT
|
4 WEEKS AFTER FERTILISATION |
1. HEART FORMSAND STARTS TO BEAT. 2. BRAIN DEVELOPS 3. UMBILICAL CORD FORMS.
|
|
|
1. INTERNAL ORGANS START TO FORM. 2. LIMBS START TO FORM. (EMBRYO |
|
|
1. EYES BECOME VISIBLE. 2. MOUTH, NOSE AND EARS BEGIN TO |
|
|
1. TAIL 2. FACE 3. MAJOR 4. OVARIES 5. BONE REPLACES CARTILAGE. 6. THE EMBRYO IS NOW CALLED A |
|
|
1. BONE GROWTH CONTINUES TO REPLACE 2. NERVES AND MUSCLES COORDINATE 3. THUMB SUCKING AND KICKING BEGIN. 4. MILK (BABY) TEETH FORM. 5. FOETUS TAKES AMNIOTIC FLUID INTO 6. EXTERNAL SEX ORGANS CLEARLY |
The Gestation period is the length of time from fertilisation to birth. In humans it is generally 266 days (38 weeks/9months).
BIRTH
1. The placenta stops producing progesterone. This causes the walls of the uterus to contract.
2. Oxytocin is produced by the pituitary gland. This hormone causes contractions of the uterine muscle. This is the beginning of labour.
3. There are 3 stages of labour:
a. Stage 1: The contractions push the foetus down toward the cervix. The membrane around the foetus (amnion) breaks. The amniotic fluid is released through the vagina.
b. Stage 2: The cervix dilates (widens) and the foetus is pushed out through the cervix and vagina. At this time the umbilical cord is cut.
c. Stage 3: The placenta and foetal membrane (afterbirth) are released through the vagina.
LACTATION
Lactation is the secretion of milk by the mammary glands of the mother. Colostrum is a thick yellow fluid produced during the first few days. It is low in fat and sugar but rich in minerals, protein, and antibodies.
Prolactin is a hormone produced by the pituitary gland. This hormone stimulates milk production. The suckling of a baby at the breast stimulates the mothers pituitary to release prolactin. When breast feeding stops the mother stops secreting prolactin and therefore stops producing milk. Suckling also stimulates the pituitary to secrete oxytocin. Oxytocin causes the milk ducts to contract ejecting the milk from the breast.
BENEFITS OF BREAST FEEDING
Human milk has a lot of advantages for the babys growth and development. Human milk is nutritionally balanced for a developing human baby. It also contains a wide variety of beneficial chemicals that include mothers antibodies. These antibodies protect the child against common pathogens. Human milk also contains chemicals favourable for brain growth and development. Human milk also encourages the growth of mutualistic bacteria in the large intestine.
CONTRACEPTION
Contraception is the deliberate prevention of fertilisation. There are 4 methods:
1. Natural contraception:
a. Abstinence: No sexual intercourse. 0% failure rate.
b. Temporary abstinence: No sexual intercourse during the most fertile period of the menstrual cycle. 24% failure rate.
c. Withdrawal: The penis is removed from the vagina before ejaculation. 25% failure rate.
2. Mechanical contraception:
a. Condom: This is a thin impermeable sheath covering the penis. Semen cannot be deposited in the vagina. 10% failure rate.
b. Vasectomy: The cutting, sealing or tying off the sperm ducts. Sperm will not be in the semen. 0.4% failure.
c. Cervix Barriers: diaphragm or cap These prevent sperm entering the uterus. 15% failure rate.
d. Intrauterine Devices (IUD): These are plastic or metal loops or coils that prevent implantation. 5% failure rate.
3. Chemical contraception:
a. Spermicides: These chemicals are placed in the vagina to kill sperm. 20% failure rate.
b. Oral contraceptive pill: Contain hormones such as progesterone and oestrogen that prevent ovulation as the follicles do not mature. 6% failure rate.
4. Surgical contraception:
a. Tubal ligation: The Fallopian tubes are cut and sealed preventing sperm and egg cells meeting. 0.4% failure rate.
b. Vasectomy: The vas deferens (sperm duct) is cut. Sperm is not present in the semen.
The % failure rate is the number of sexually active females out of a hundred who will become pregnant within a year.
Take a break from studying and play some cards! Read the reviews of the top Texas Holdem poker sites at iTexasHoldem.
Related Courses
Submit your review | |
Never given a review on a website as long as I live..except now...but I just want to say thank you for these notes....they are really helpful.